The subperiosteal implant procedure is an advanced solution for patients with severe bone atrophy who are not candidates for traditional dental implants. This approach relies on modern digital workflows, combining high-precision imaging, customized design, and carefully planned surgical protocols to achieve predictable outcomes.
From diagnosis to final restoration, each step is designed to maximize safety, stability, and long-term success.
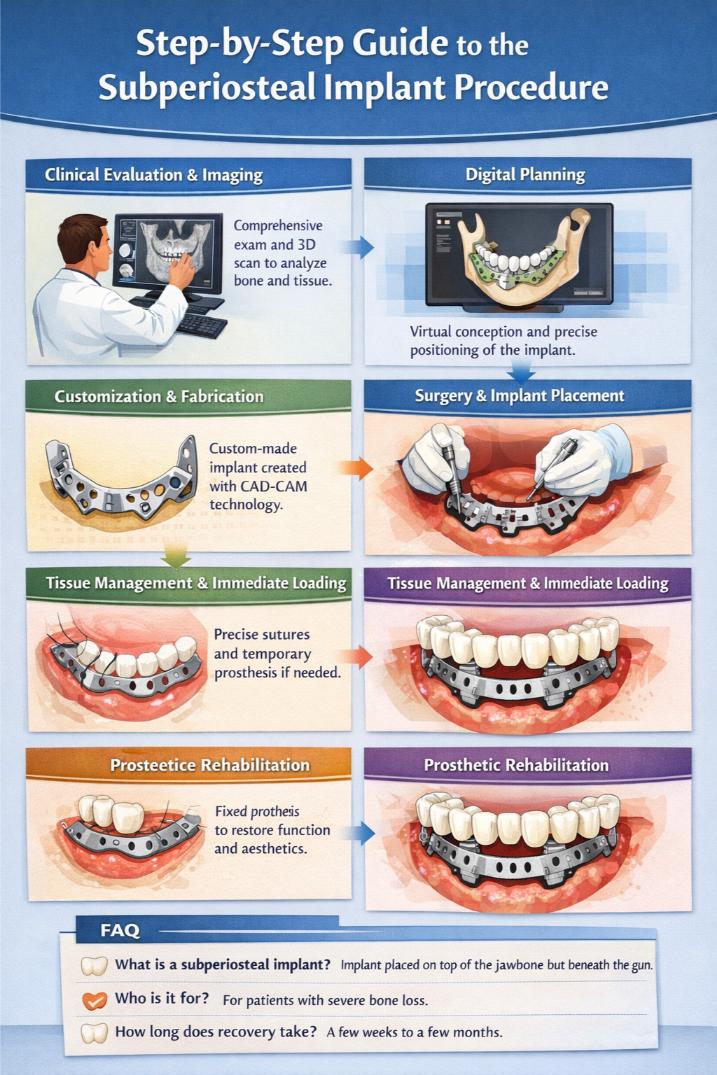
- 1 Clinical Evaluation and Diagnostic Imaging
- 2 Tissue Assessment and Digital Planning
- 3 Examination and Planning Phases
- 4 Customization and Design of the Implant
- 5 The Surgical Procedure: Step-by-Step
- 6 Placement of the Subperiosteal Frame
- 7 Soft Tissue Management and Immediate Function
- 8 Postoperative Care and Prosthetic Rehabilitation
- 9 FAQ
Clinical Evaluation and Diagnostic Imaging
The process begins with a comprehensive clinical evaluation. The clinician conducts a detailed patient interview and reviews medical history to assess potential risks and determine suitability for prosthetic rehabilitation.
Both intraoral and extraoral examinations are essential. These help evaluate soft tissue conditions and identify any pathology that could compromise the procedure.
A key component at this stage is advanced diagnostic imaging. Techniques such as CT scans, CBCT, or 3D imaging provide highly detailed views of bone contours and density. These scans reveal anatomical constraints—such as sinus proximity or nerve pathways—offering critical insights for the customization of the implant.
Tissue Assessment and Digital Planning
A thorough evaluation of both hard and soft tissues is essential for accurate case selection.
Bone analysis focuses on:
- contours and undercuts
- thickness variations
- structural defects
This ensures that the implant framework will fit precisely onto the jawbone. Bone density is also assessed to anticipate stability and determine whether additional support is needed.
Soft tissue evaluation includes examining keratinized mucosa and tissue mobility. These factors can significantly influence healing and help predict potential risks such as exposure, inflammation, or delayed recovery.
Examination and Planning Phases
Digital workflows have transformed implant planning. Specialized software allows clinicians to overlay imaging data onto virtual models, enabling precise simulation of implant positioning.
This step helps identify critical anatomical structures and ensures that the surgical plan avoids sensitive areas.
Collaboration between the surgeon, prosthodontist, and dental technician begins early. By sharing digital files and aligning on patient-specific needs, the team establishes a coordinated treatment strategy that guides every subsequent phase.
Customization and Design of the Implant
The next stage involves the design of a fully customized implant.
Using CAD-CAM technology, a patient-specific framework is created to match the exact geometry of the jawbone. This level of precision reduces micromovements and enhances primary stability.
The clinician carefully reviews the virtual design before production, ensuring all anatomical and prosthetic considerations are respected.
For a deeper understanding of modern approaches and technologies used in this field, additional insights can be found on websites such as Subperiosteal.
Once validated, the implan (typically made from titanium or cobalt-chromium) is manufactured to ensure biocompatibility and long-term durability.
The Surgical Procedure: Step-by-Step
On the day of surgery, the procedure follows a structured and carefully planned protocol.
Patient preparation includes strict antiseptic measures to minimize infection risks. Depending on the case, local or general anesthesia is administered to ensure patient comfort.
The surgeon then performs a precise incision to expose the jawbone, following the preoperative digital plan. Care is taken to minimize trauma and allow for tension-free closure.
Placement of the Subperiosteal Frame
Once the bone is exposed, the custom-made implant is positioned over the alveolar ridge.
The framework is secured using mini-screws or other fixation methods defined during planning. Accurate adaptation ensures immediate primary stability and reduces micromovement.
Intraoperative verification is critical. The clinician confirms that the implant does not interfere with nerves, blood vessels, or sinus cavities before proceeding to closure.
Soft Tissue Management and Immediate Function
Soft tissue handling plays a crucial role in the success of the procedure.
Flaps are repositioned and sutured carefully to avoid tension, promoting optimal healing and reducing the risk of complications such as dehiscence or infection.
In selected cases, immediate loading may be possible. Temporary prostheses can be placed shortly after surgery, allowing patients to regain both function and aesthetics within a short timeframe.
Postoperative Care and Prosthetic Rehabilitation
The postoperative phase is essential for long-term success.
Patients undergo a monitored healing period, supported by personalized hygiene protocols. Soft tissues gradually adapt to the new structure, while any signs of inflammation or instability are addressed promptly.
Once healing is complete, prosthetic rehabilitation begins. Fixed bridges or hybrid prostheses are designed to restore full function and natural appearance.
Accurate impressions or digital scans ensure a precise fit, while regular follow-ups help maintain stability and patient satisfaction over time.
FAQ
What is a subperiosteal implant ?
A subperiosteal implant is a custom-made framework placed on top of the jawbone but beneath the gum tissue, designed for patients with insufficient bone volume for traditional implants.
Who is a good candidate for this procedure ?
Patients with severe bone atrophy who cannot undergo bone grafting or prefer an alternative solution may be suitable candidates.
Is the procedure painful ?
The surgery is performed under anesthesia, and postoperative discomfort is typically manageable with standard care and medication.
How long does recovery take ?
Initial healing usually takes a few weeks, while full integration and prosthetic rehabilitation may take several months depending on the case.
From initial diagnosis to digital planning and final restoration, the subperiosteal implant procedure represents a structured and highly precise approach to complex dental rehabilitation.
By combining advanced imaging, customized design, and interdisciplinary collaboration, this technique offers a reliable solution for cases once considered difficult to treat—transforming clinical limitations into predictable outcomes.
